One Death. Four Lives
He agreed to a posthumous transplant of his mother’s organs because once he himself had needed someone else’s heart.
While her son was receiving a heart transplant, at a nearby hospital a priest was blessing her daughter who would not make it any longer without a liver transplant.
She got a new liver by chance—she was in the hospital at just the right time.
“February 10, 2021 is the most dramatic day in Ukrainian transplantology,” says the author of this text, Iryna Zaslavets. And we believe her. Iryna is a TV journalist and the founder of the iDonor All-Ukrainian Donation Platform. Ten years ago, she underwent a transplant herself and now promotes organ donation and is helping effect titanic changes in the healthcare system. Iryna has witnessed almost all organ transplant surgeries that have been carried out in Ukraine in recent years. She told a story about one of them exclusively for Reporters.

February 6. A 45-year-old woman is brought to the Clinical Emergency Care Hospital in Lviv. She has suffered an aneurysm rupture and cerebral hemorrhage. Doctors try to “fix” the vessel, but a blood clot breaks off and another rupture occurs. The patient suffers a cerebral oedema. Then follows another surgery and the realization: there is no chance of survival.
February 9. Lviv. The middle of the day. The medical case conference pronounces the death of the brain. After a difficult conversation, her husband and mother agree to a posthumous donation. So do her pregnant daughter and 17-year-old son. The family knows what it means to wait for a donor organ. The youngest son of the donor was born with multiple heart defects, and the doctors warned them that their son would not survive without a transplant. Back then it was tantamount to death, because at that time no heart had been transplanted into a child in Ukraine. But, fortunately, the boy survived—after several surgeries his heart was successfully recovered.
The evening of February 9. Kyiv. Due to heavy snowfall, the roads in the country are impassable. I get on the train with doctors from the Heart Institute and the Shalimov Institute of Surgery and Transplantology. We reach Lviv the next morning.
February 10. 5:30 am
It is still dark outside. Doctors and nurses are lining up along the corridor. Everyone has come when they heard that the person whose death will save four lives will now be taken to the operating room down this corridor.
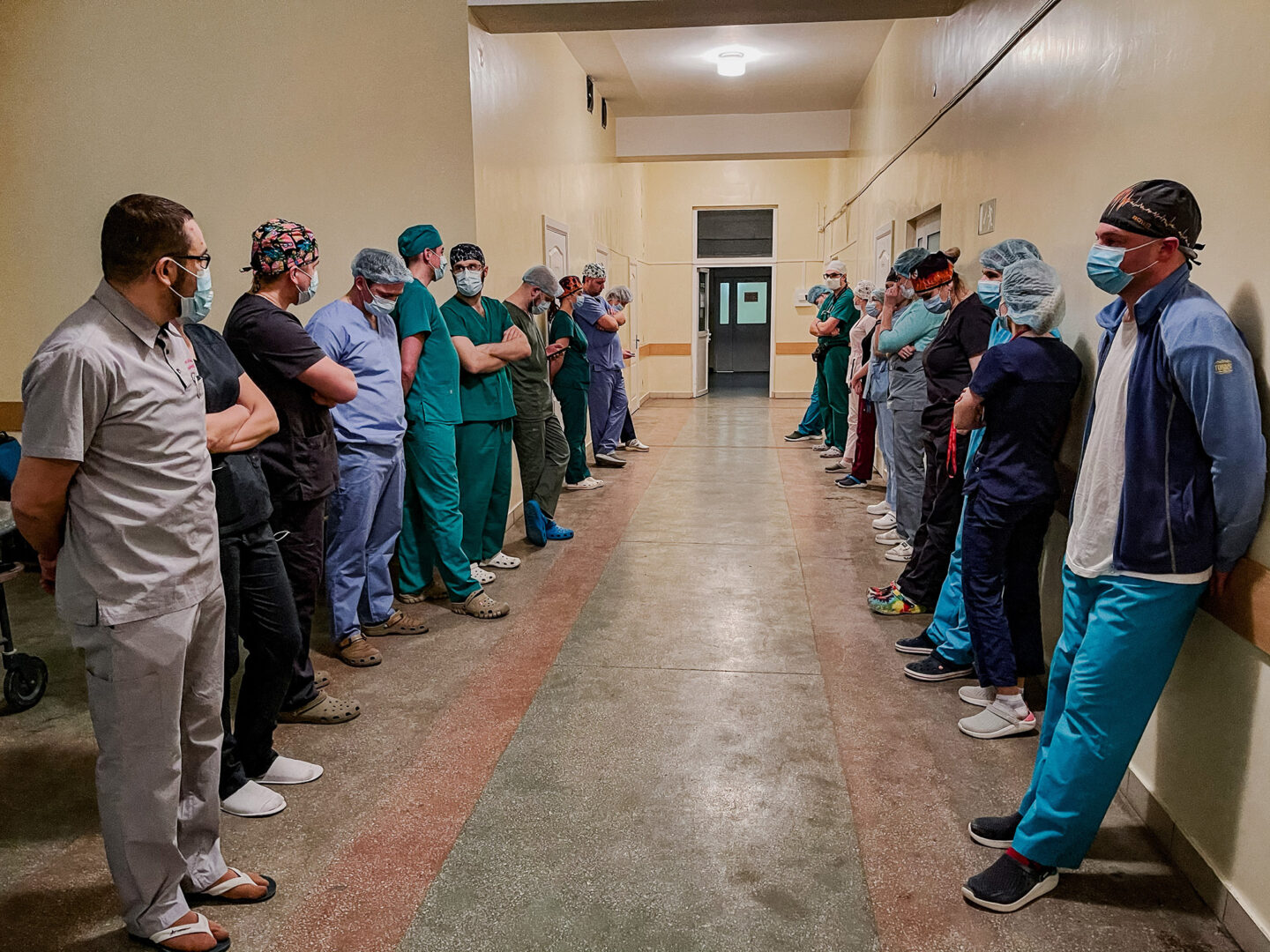
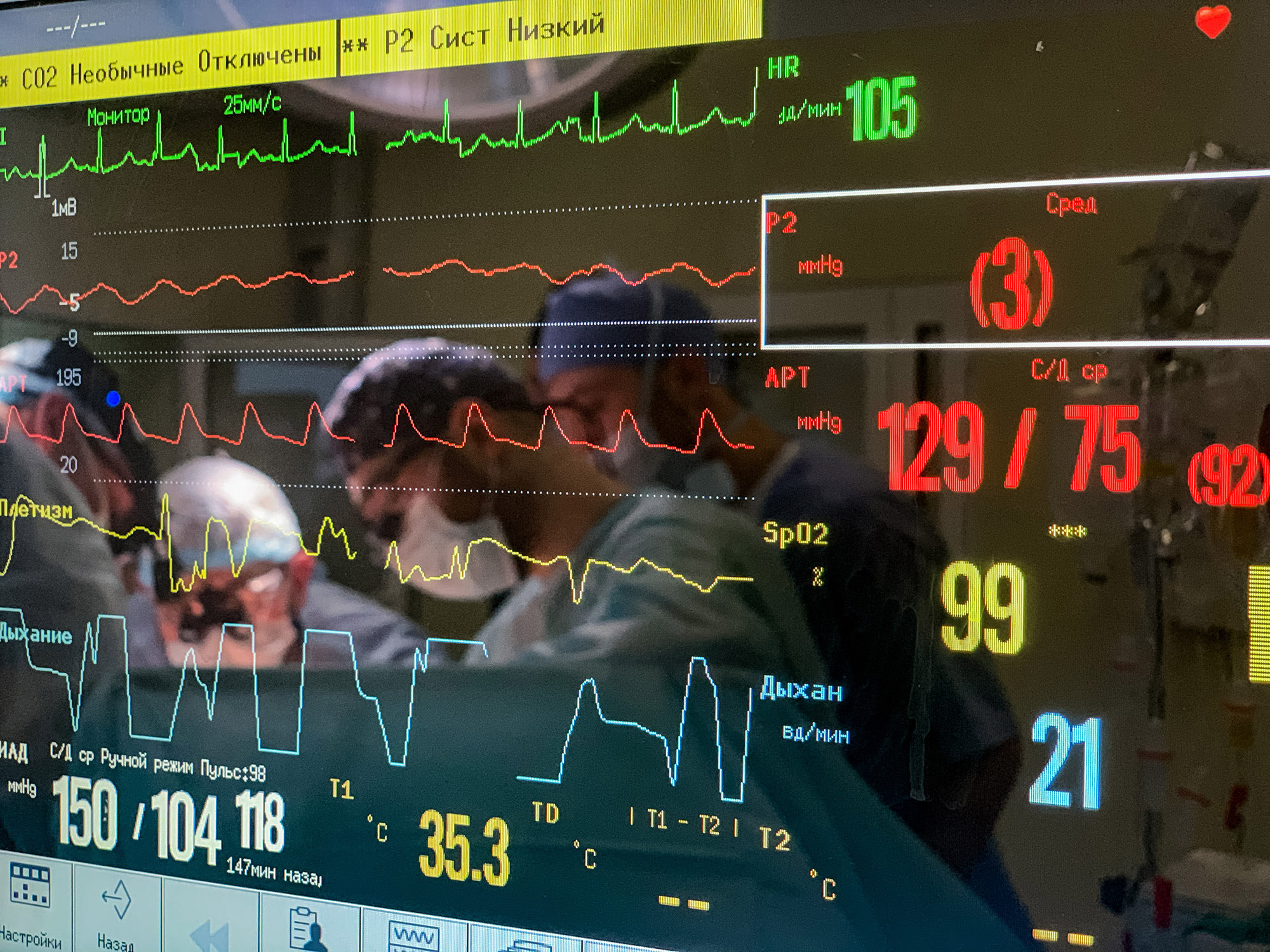
People bow their heads. The monitor reporting on the patient’s condition is beeping loudly. The head of the resuscitation department is pushing the stretcher on which the woman is lying while pumping an oxygen bag. Although the donor’s brain has died, she will keep on breathing for a while thanks to that bag and life support equipment.
Shivers go down my back. This “corridor of honor” is a thank you to the donor for the highest manifestation of sacrifice and love for thy neighbor. Love to the very end.
5:45 am
Up in a ward on the fourth floor, the sound of a heartbeat can be heard. The monitor shows an organ three times the size of a healthy one. A young man lies on the hospital bed confused, even though he says: “I am not afraid.” Vasyl comes from a village in the Lviv region, and the day before yesterday he turned 22. He has been living with a congenital heart disease, but found out about it only three years ago when he contracted the flu and suffered from complications. The donor organ is the only thing that can save his life.
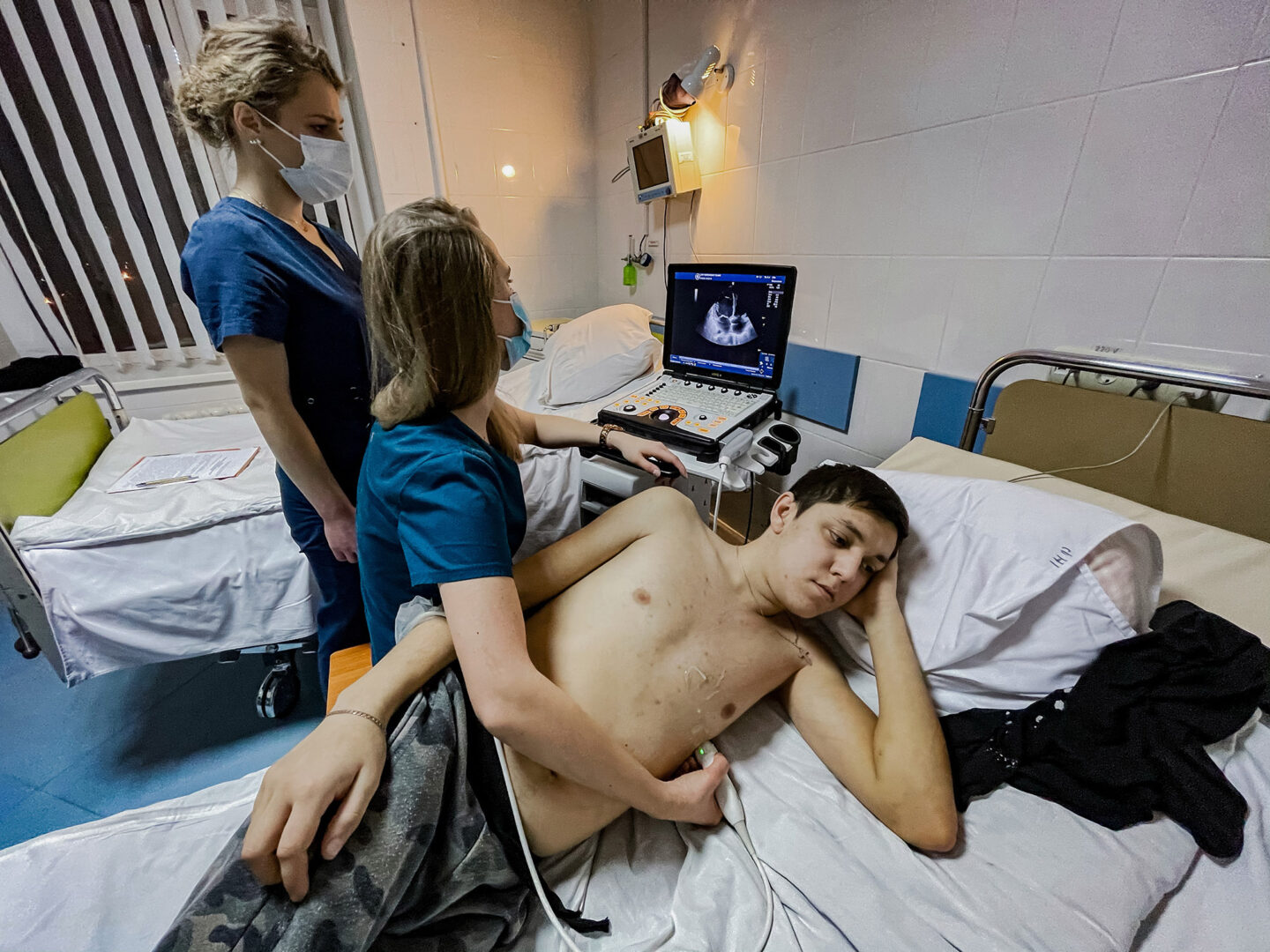
Vasyl is alone in the ward. The doctors cheer him up, but his mother is not around. She is in another hospital in Lviv, with her 35-year-old daughter. Three years ago, she was also diagnosed with a terrible disease—autoimmune hepatitis and liver cirrhosis. A transplant could be the young woman’s only chance at life, as in the case of her brother, but no one told her about it. Until her state became critical some days ago. She is already unconscious. The mother called a priest so that he would bless her daughter. The doctors said it was over.
“I am not worried about myself, I am worried about my sister,” Vasyl says. He is taken for surgery not knowing whether he will ever see her again.
6:30 am
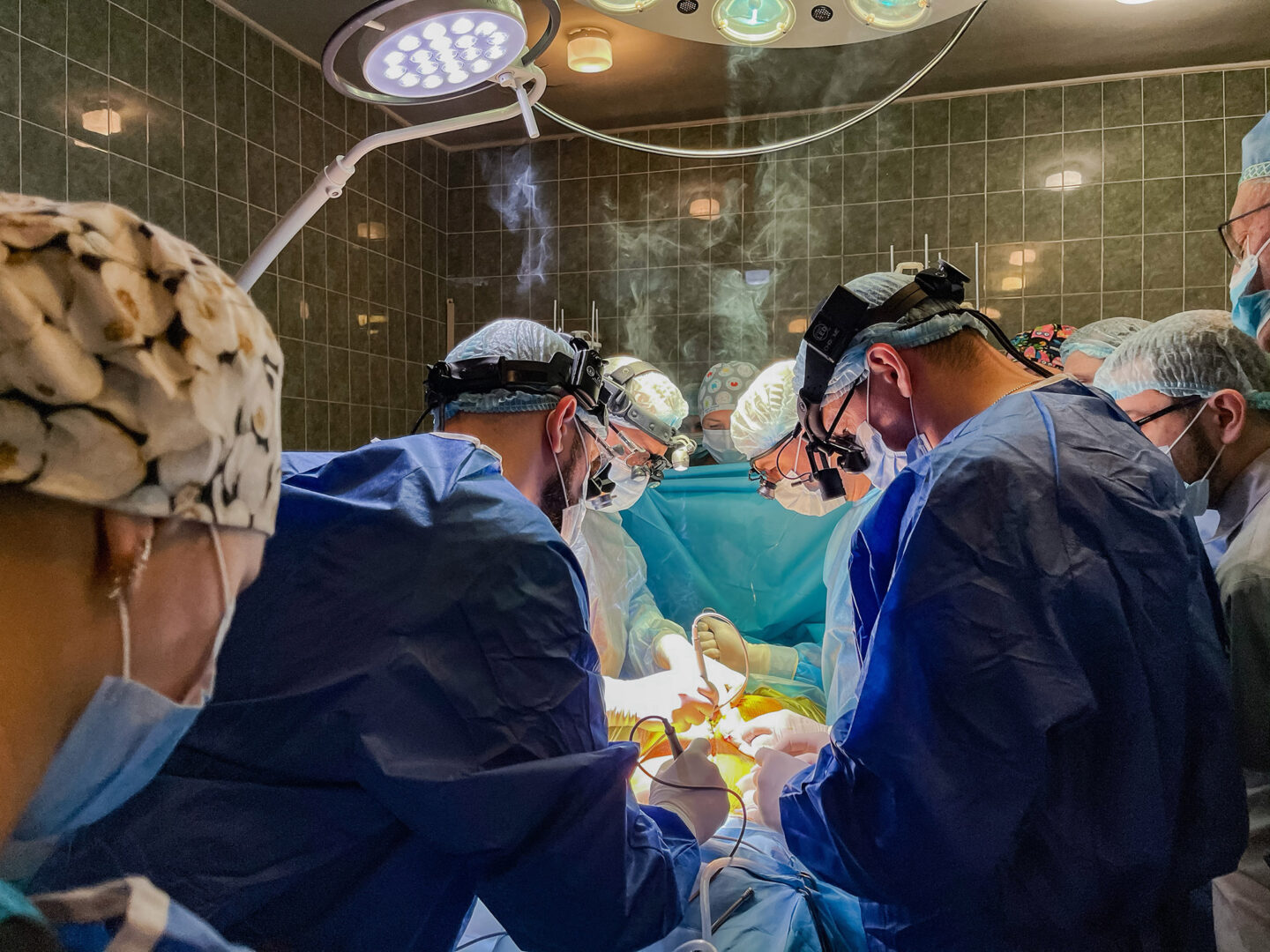
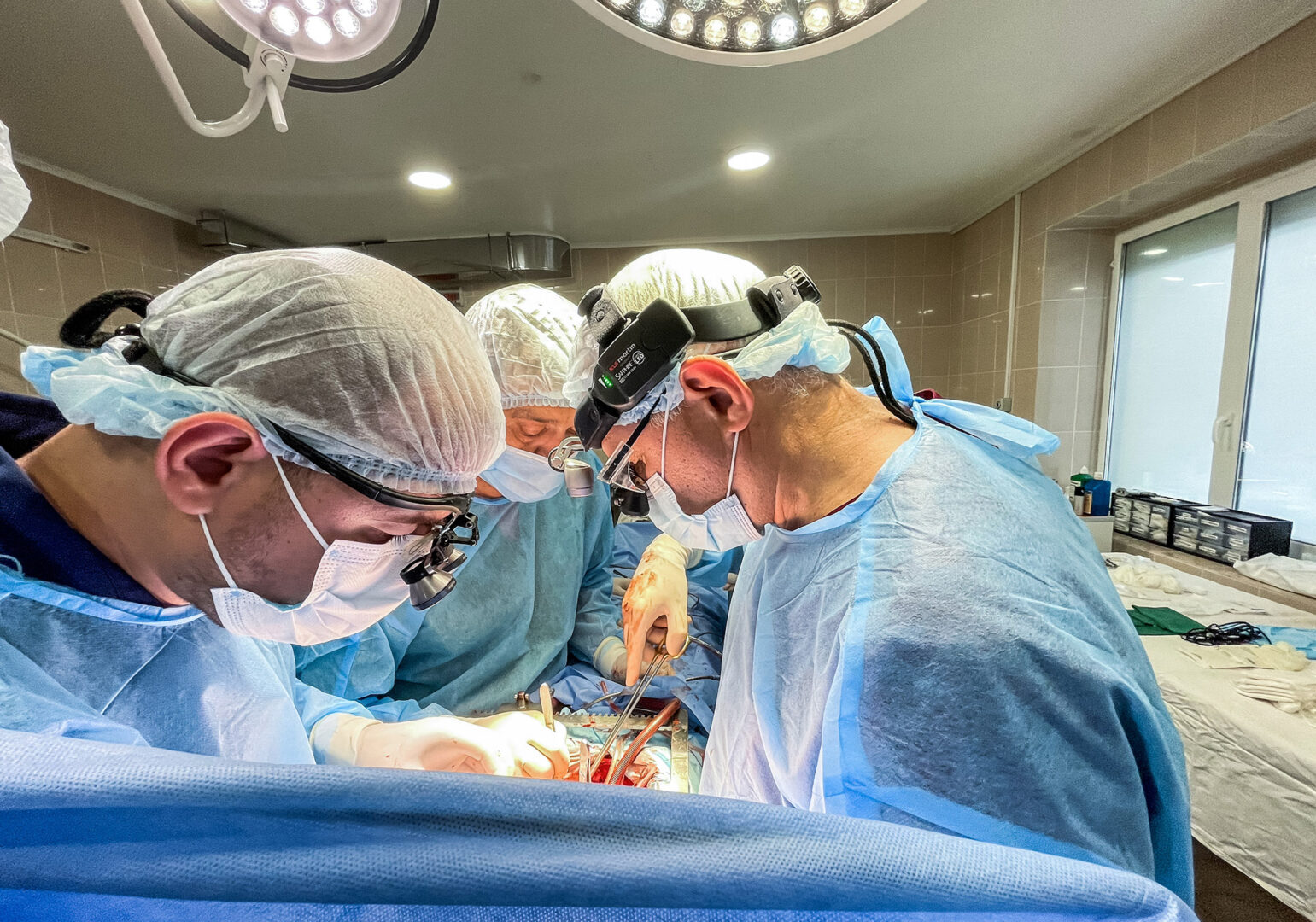
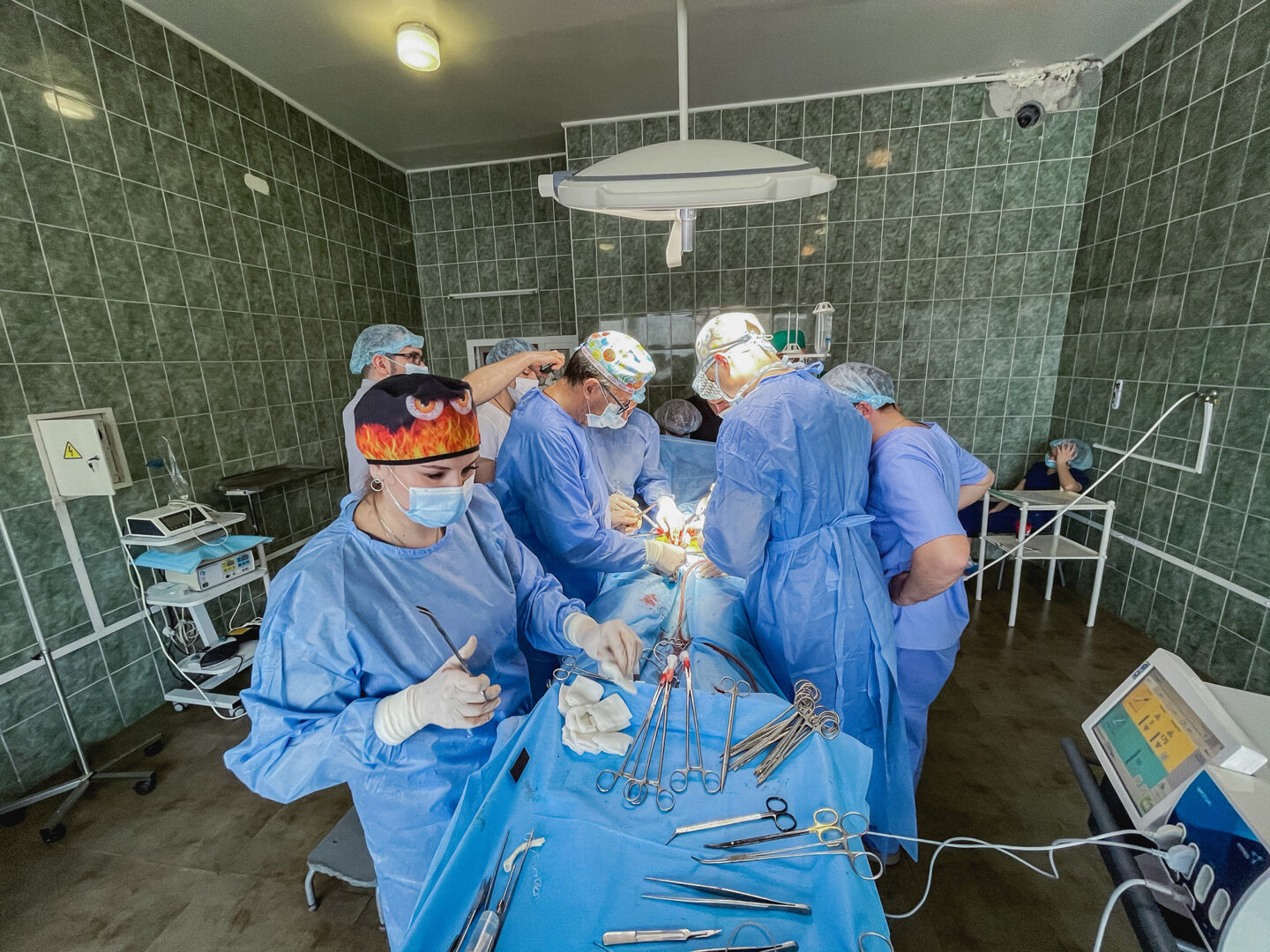
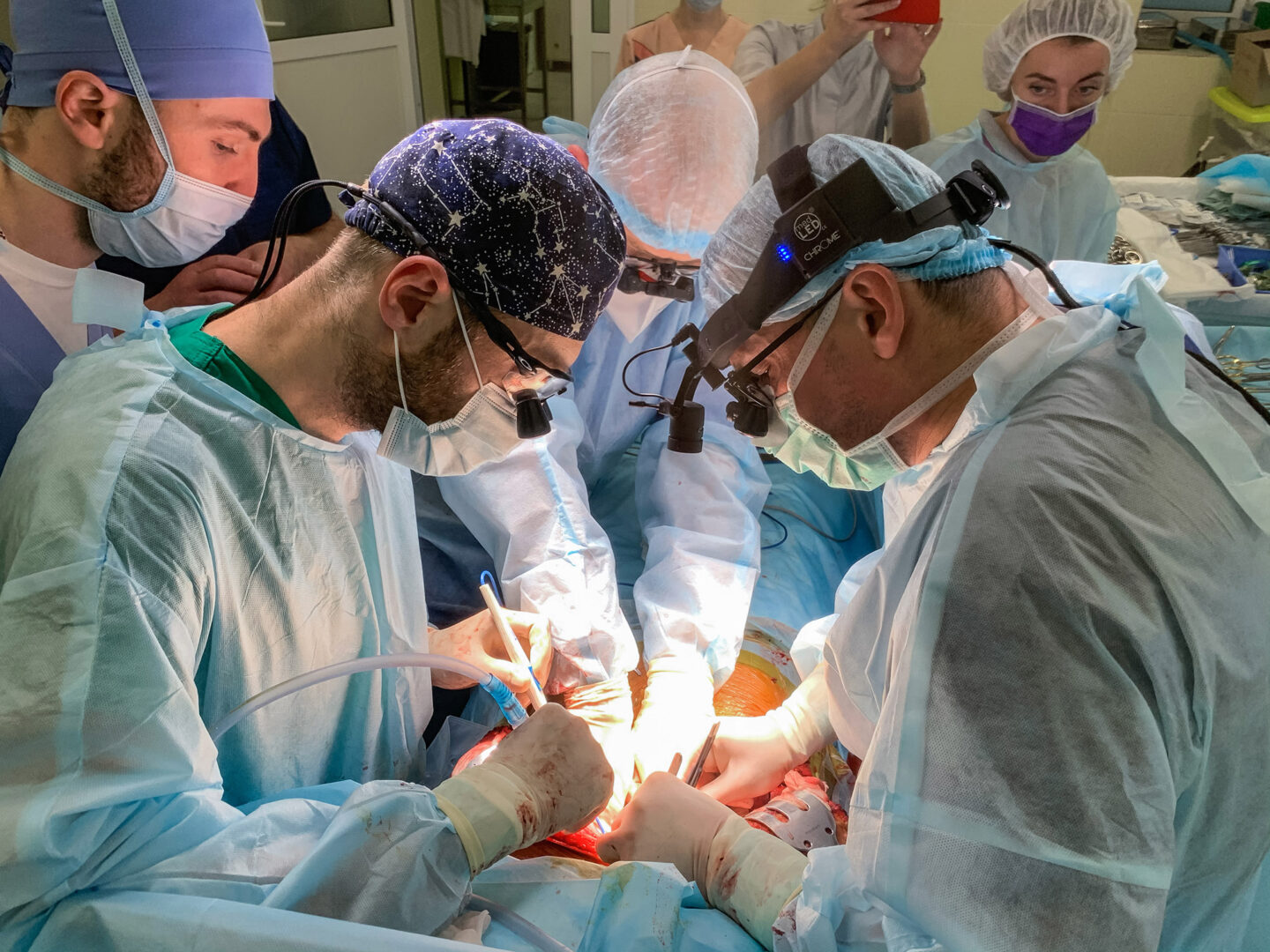
The operating room. Monitors are beeping, ice is being broken to cool the organs, drips and lights are being set up. It is like a beehive, with thirty or forty people in the room. All of them are needed to conduct a multi-organ harvest: the heart, the liver, and two kidneys.
The surgeons put their gloves on and approach the table. And suddenly a silence descends that is even louder than the sounds of the monitors. Before making the first incision, the doctor conducting the operation, Borys Todurov, traditionally says:
“Let us honor the person who in death is giving her organs in order to save others.”
A few seconds of heavy silence follow.
“With God’s blessing! Let us begin.”
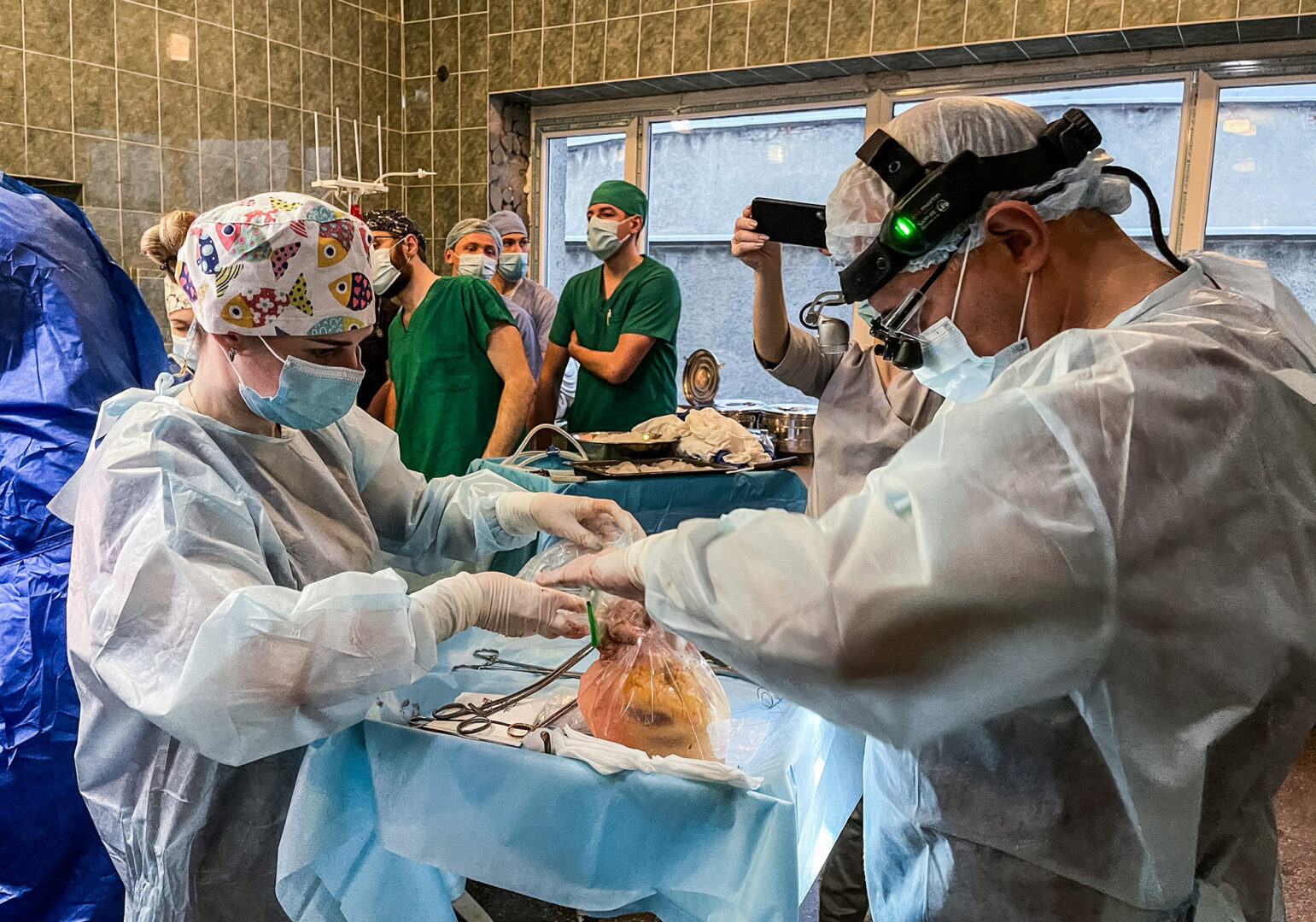
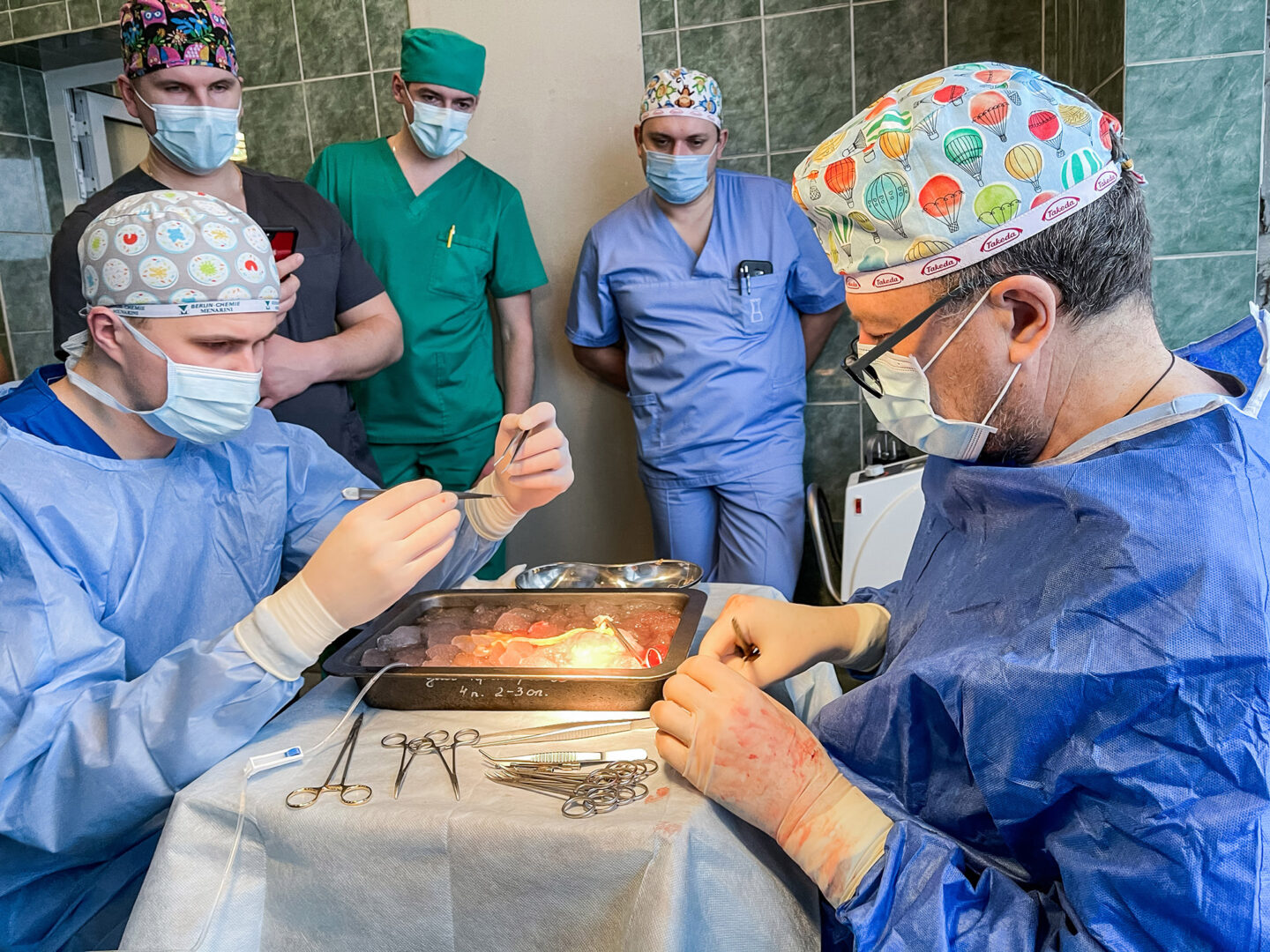
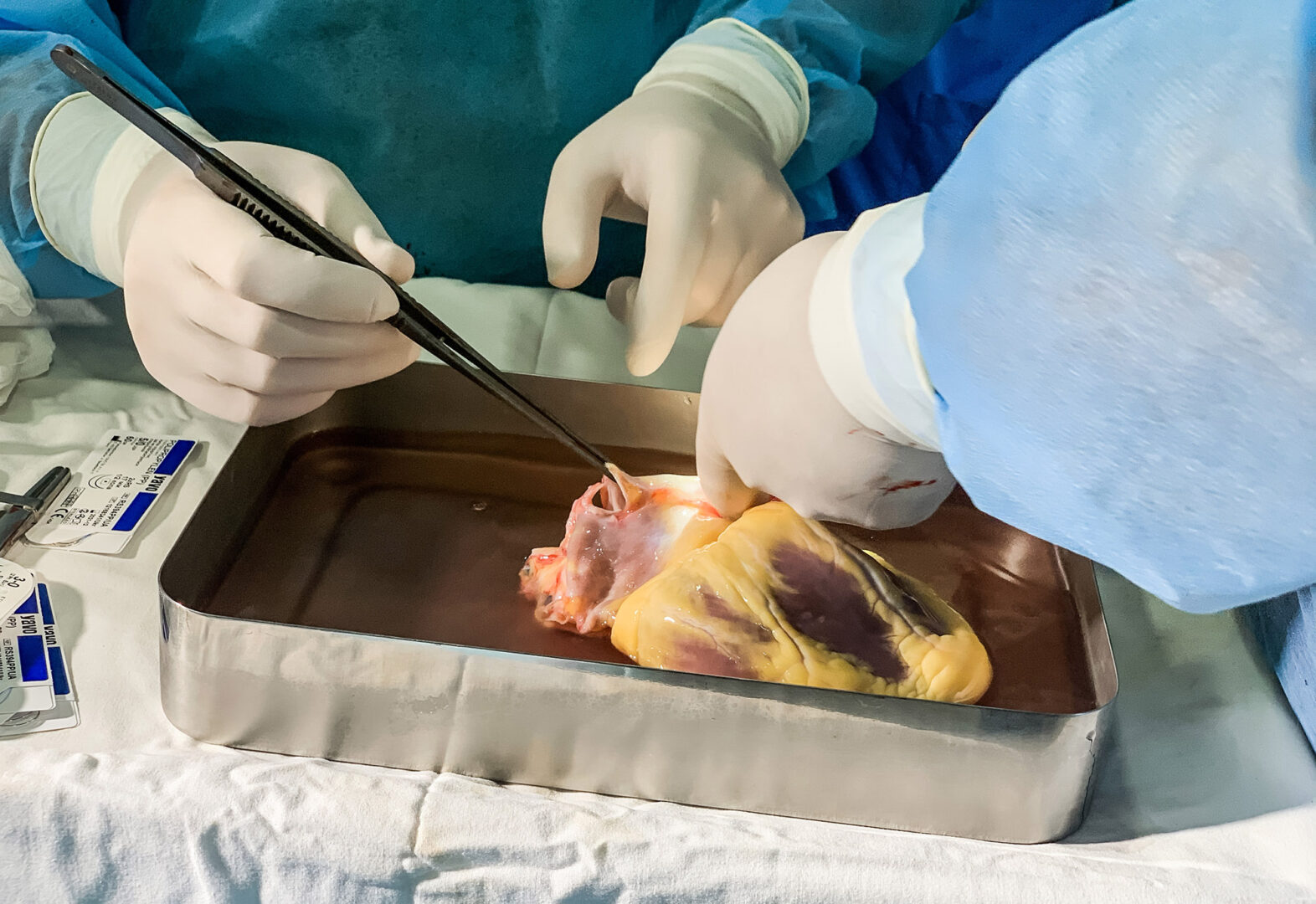
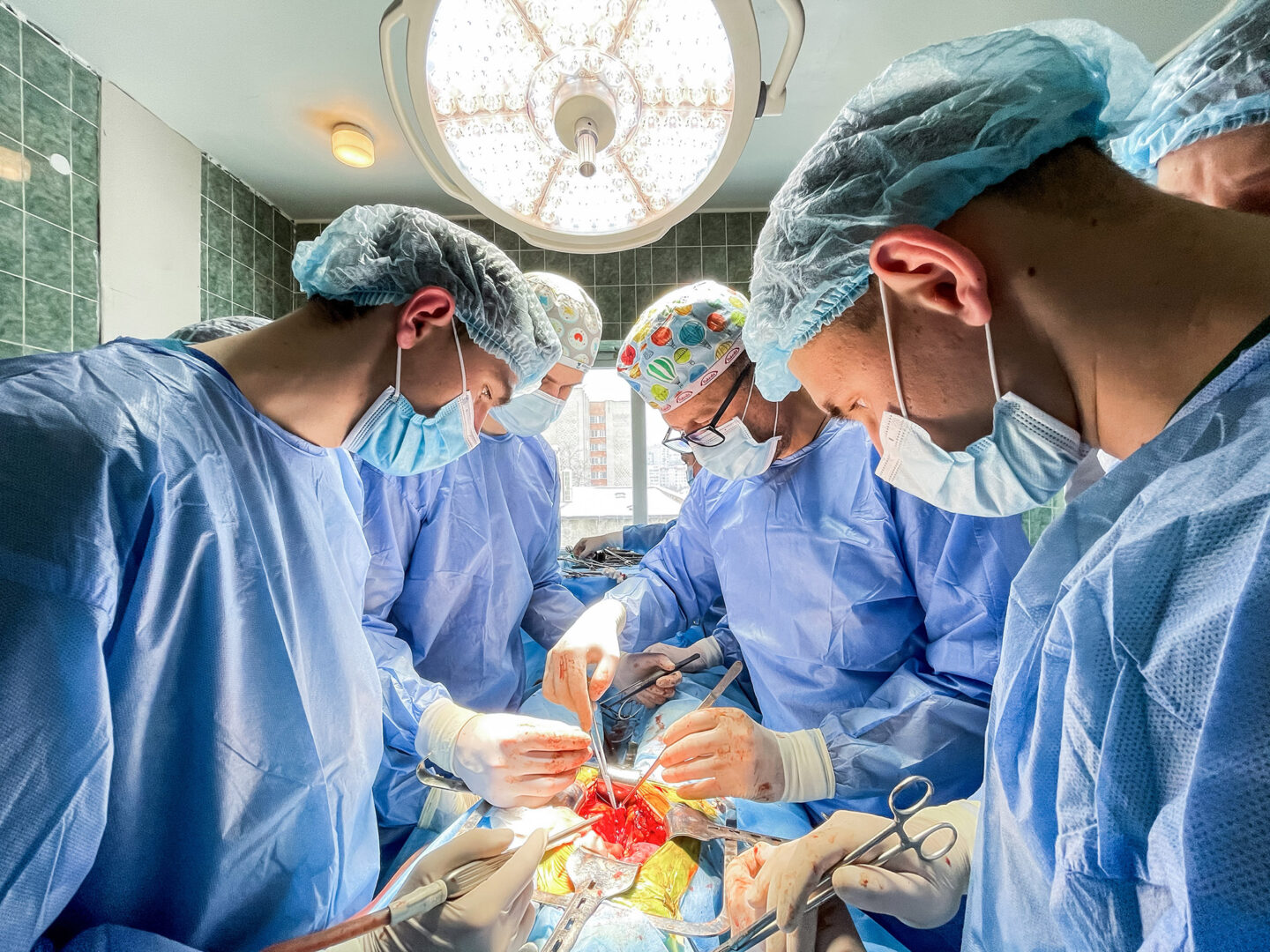
The first incision is made, the chest is opened, and in turn the heart, the liver and the kidneys are placed in transplant boxes. Each in its own. They will all be transplanted synchronously.
7:50 am
I am the first to run to the operating room where the heart gets taken. Everyone must act very quickly, because the organ can only survive outside of the human body for four hours. This should be enough time for the heart to start beating in Vasyl’s chest. If they do not make it in time—the organ will be permanently damaged and will no longer be able to function.
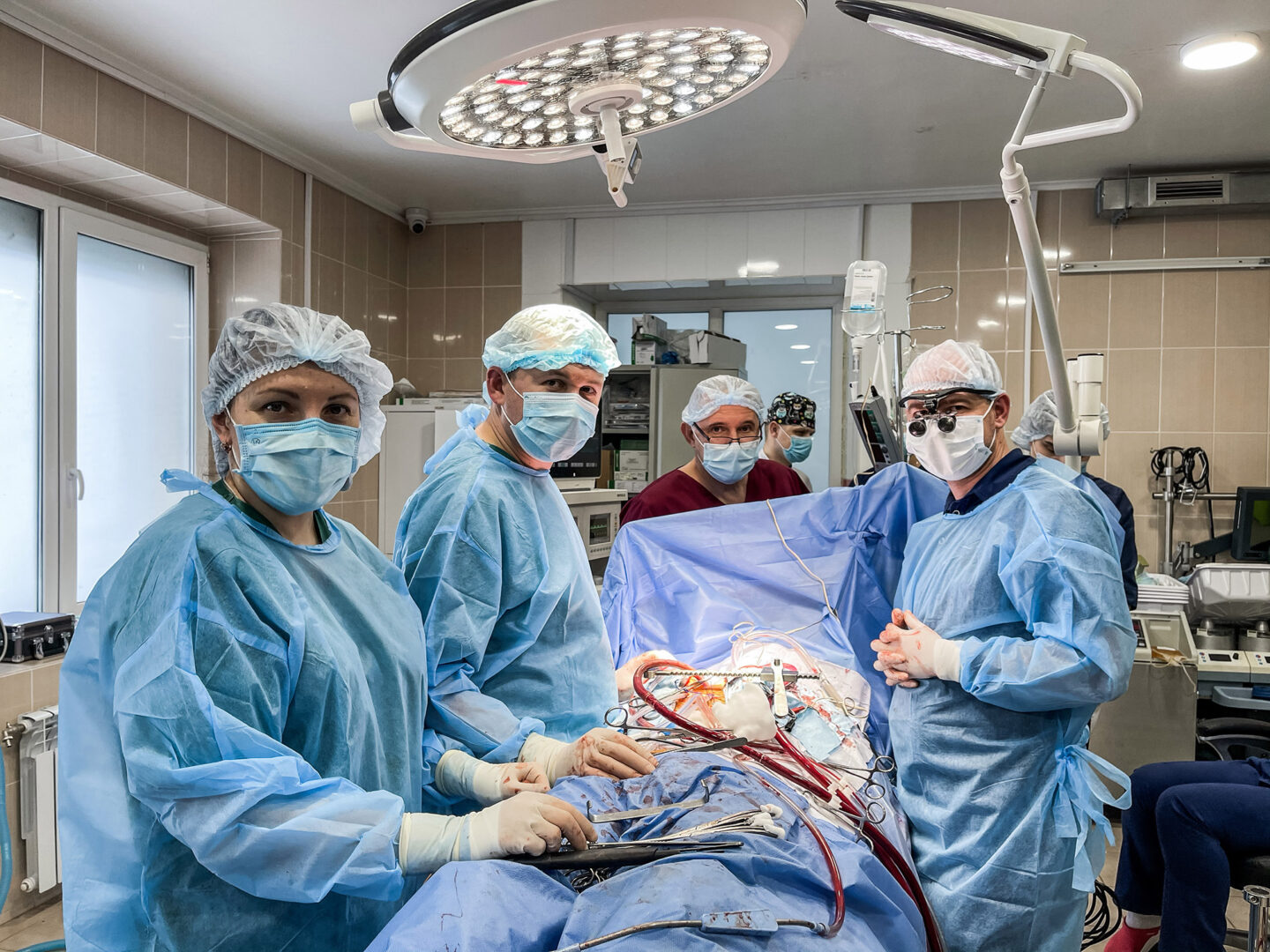
The operating room where the heart will be transplanted is located three floors below. While I make my way down, the doctors are already at the table. The anaesthesiologists are by their side. The ventricular assist device is quietly doing its job.
A moment later and I can see Vasyl’s worn-out heart in the hands of the cardiac surgeon. The disease made the muscle swell like a ball, almost losing its ability to contract. Without a transplant, the boy would die within a year, provided he did not contract any infections or colds, which could easily provoke acute heart failure. Having such a heart in your chest is like carrying a bomb that can detonate at any time.
And while the “old” heart is making its last contractions on the surgical nurse’s table, the cardiac surgeons place a healthy, elastic muscle in the young man’s chest. An hour later it will make its first beat. The straight line on the monitor will be replaced by a cardiogram. I will call it magic, but the doctors will routinely object: they call it “professionalism.”
There is an hour and a half of work ahead, and then Vasyl will be transferred to the resuscitation department. By that time, his mother Halia should have arrived. Her eldest daughter took her place by her sister’s side, and Halia is already in the shuttle bus.
“I am going as fast as I can,” she tells me on the phone. And she is even afraid to ask how her son is doing. I don’t say anything either. It’s the doctors’ job.
10:00 am
I hurry up to the fourth floor. The hospital is huge. I’ve walked 5,000 steps here since dawn. In the furthest operating room, transplantologists are suturing the kidney. Their patient is a woman. I can see her manicured fingers from under the blue sterile covers. Oksana lives in Lviv, she is 36. Her kidneys failed seven months ago, and she has been on dialysis ever since.
Everyone present is frozen, waiting to see how her body reacts. In an instant, yellow fluid starts dripping into the urinary catheter. I want to shout “hurray!”, and I notice a satisfied smile on the doctors’ faces: they did it! People on dialysis do not urinate, so doctors and patients with kidney failure are very happy to see urine.
The only thing left here is stitching her up, so I move to the next hall.
10:25 am
Anaesthesiologists are administering anaesthesia to 34-year-old Yaroslav. He has been suffering from kidney failure for the past 25 years. Yet, he has joy in his life—his wife and two daughters: the oldest is 1.7 years old, and the youngest 7 months old. When he talks about them, his eyes fill with tears. His name was added to the national transplant waiting list a little over a month ago.
“I hope it all works out,” I tell him before running back to the ground floor. Vasyl’s mother Halyna has arrived. My phone shows that I have now done 8,000 steps.
10:50 am
A woman is standing in front of the resuscitation department. Although she is trying to control herself, it is evident that she is afraid. Her morning as a mother has been hell on earth: one child is on her deathbed, another—undergoing complex surgery.
“Everything went well, your son. . .,” starts cardiac surgeon Roman Domashych, who goes out to meet her, but Halyna rushes to embrace him.

“Thank you! Thank you so much!” she can barely control herself. “And I would like to thank the donor’s family for my son’s life! I understand that it is very painful for them, but I am so grateful. If my daughter’s heart was healthy, I would give it away to save someone’s life,” she says emotionally.
For just a few seconds, the mother is allowed to look through the doors of the intensive care unit where Vasyl has already been taken. Halyna covers her mouth to keep herself from crying. Her son will live.
But her daughter will not. Just an hour ago, the doctors said they were sending her back home to live out her last days.
“What is her blood type?” the doctor asks.
“A (II) Rh+.”
The doctor looks down. If his colleagues had referred the woman for a transplant in time and she had been treated, she and her brother could have both received a new organ today—the recipient, who was being prepared to receive the liver, refused to undergo surgery. So right now, in this hospital, there is an organ that could match her daughter, but in her condition transplantation is contraindicated.
The doctor does not say this out loud, though—he does not want to break the mother’s heart even more.
Noon
There are more miracles to be had today. Although after such twists and turns it seems hard to believe. Once out of the human body, the liver can survive up to 12 hours. Therefore, after one patient rejected it, doctors had to quickly find and prepare another person who needed such an operation. And they found her right there, in the hospital!
Halyna is 48 and is from the Lviv region. For three years she has been living with a liver affected by cirrhosis and the doctors’ conclusion that only an organ transplant could save her. Yet, the woman was not on the list at the Transplant Center.
A month ago, Halyna became very ill—she suffered an oesophageal-gastric bleeding. With this diagnosis, the woman was admitted to the Lviv Emergency Care Hospital. Now she has returned for additional treatment and, in a manner of speaking, caught the eye of the transplantologists.
It took Halyna forty minutes to give her consent for the surgery. After the examination, her data was entered into the Unified State Transplant System and it was confirmed: the organ is a match for her.
While I am writing this, Halyna is undergoing surgery. They are in hour four. The donor liver is currently being sutured. Everything is going according to plan.
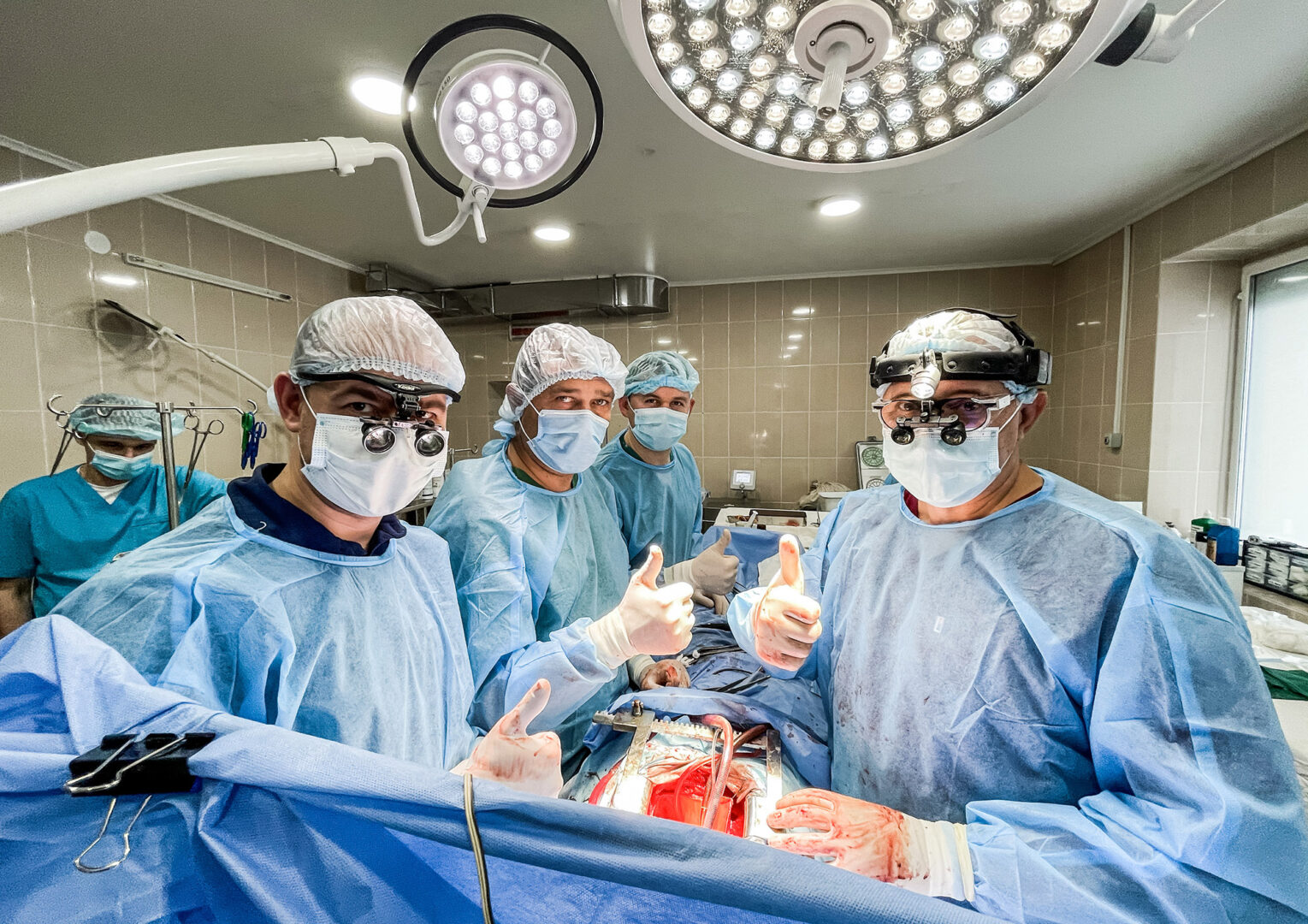
Yaroslav and Oksana with their donor kidneys and Vasyl with his new heart are also in a stable condition. Ahead is the process of recovery, and then, I hope, a long and healthy, happy life.
“Organ transplantation offers thousands of people a new chance. And we want to give Ukrainians this chance,” said Oleh Samchuk, Executive Director of the Lviv Emergency Care Hospital, in July when the first post-mortem transplantation was performed there.
This day has shown us once again that our doctors have a real knack for it.

[This story was created with support of the Royal Norwegian Embassy in Ukraine. The views and opinions expressed in this publication are those of the authors and do not necessarily reflect the official position of the Norwegian government.]
Have read to the end! What's next?
Next is a small request.
Building media in Ukraine is not an easy task. It requires special experience, knowledge and special resources. Literary reportage is also one of the most expensive genres of journalism. That's why we need your support.
We have no investors or "friendly politicians" - we’ve always been independent. The only dependence we would like to have is dependence on educated and caring readers. We invite you to support us on Patreon, so we could create more valuable things with your help.
Reports119
More